Allergy Symptoms in Babies
Symptoms of Food Allergies in Babies
Symptoms vary and range from mild to severe. Generally, the severity of a reaction is judged by how many symptoms are present and the severity of those symptoms.
If you think baby is having an allergic reaction, call emergency services immediately.
Symptoms of Allergic Reaction in Babies
Mild Reaction (includes one symptom below) |
|---|
a few isolated hives or mild itching |
itchy or runny nose |
mild nausea or vomiting once |
Severe Reaction (Anaphylaxis) (includes any symptom below, either alone or in combination) |
|---|
hives or rash that spread across the body |
swelling of the face, lips, or tongue |
repetitive vomiting or diarrhea |
shortness of breath, wheezing, stridor, hoarse cry, or repetitive cough |
drooling more than usual |
pale, ashen, bluish, or mottled skin |
sudden limpness, poor head control, or unusual sleepiness |
inconsolable crying or sudden extreme behavioral change after eating |
Mild Reaction
Includes ONE of the following (more than one is a severe reaction):
Itchy or runny nose, sneezing
Itchy mouth
A few isolated hives or mild itching
Mild nausea or gastrointestinal discomfort, or a single episode of vomiting
A mild allergic reaction involves one symptom. For example, baby might have a few isolated hives around the mouth, a runny nose, or a single episode of vomiting. If you see only one of these, stop feeding the allergen and contact your doctor or allergist for guidance.
If baby is having multiple symptoms, call emergency services immediately and request an ambulance equipped with epinephrine.


Severe Reaction
Includes any of the following, either alone or in combination:
Shortness of breath, wheezing, stridor (a whistling sound upon breathing in), repetitive cough
Excessive drooling
Pale, ashen, bluish or mottled skin
Swelling of face, lips, or tongue
Hives or rash hat spread across the body
Repetitive vomiting or diarrhea
Sudden limpness, poor head control, unusual sleepiness
Inconsolable crying or sudden extreme behavioral change after eating
A severe allergic reaction is called anaphylaxis. It involves two or more body systems at the same time, or includes any severe symptom on its own. It can progress rapidly, which is why immediate action is essential.
If baby is having any of the above symptoms, call emergency services immediately and request an ambulance equipped with epinephrine. Do not wait.
The distinction families most commonly miss: anaphylaxis does not always look dramatic at the outset. A baby who develops hives and then vomits, or who seems unusually floppy and is also coughing, is showing signs affecting more than one body system—even if no single symptom appears severe on its own. When more than one system is involved, call emergency services right away.







Delayed Reactions
Most allergic reactions occur within minutes of eating, though delayed reactions that occur several hours later are possible with FPIES, an increasingly recognized food allergy in babies and young children. It is often challenging to confirm an FPIES allergic reaction without the support of your doctor and a pediatric allergist or gastroenterologist because the most common symptoms are vomiting and diarrhea, which are common reactions to a number of childhood illnesses. Check out FPIES in Babies for more information.
A baby may not have an allergic reaction the first time they are exposed to the food, so be watchful on the second and the first few subsequent exposures. Generally, the more of the allergen consumed, the more severe the reaction is likely to be, so it is important to start small when introducing new foods and gradually work up to larger quantities served at mealtime.
Why Anaphylaxis Looks Different in Babies
Older kids can tell you when something feels wrong. They might say their throat feels tight or their heart is beating fast. Babies can't talk yet, so you have to watch for other signs. Look at their skin, their breathing, how their body moves, and how they're acting.
Early signs of a bad allergic reaction in babies can include fussiness, tiredness, or an upset stomach. The tricky part is that babies often act this way even when nothing is wrong. Pay close attention to timing: if these signs show up soon after your baby eats something, take it seriously.
It also helps to know what to look for before you introduce a new food. Many parents and caregivers don't realize baby is having a reaction until after it's over. Learning the symptoms of an allergic reaction ahead of time makes them much easier to spot.
Anaphylaxis in Infants vs. Toddlers
The Asthma and Allergy Foundation of America studied severe allergic reactions in children under three. They talked to parents and caregivers who had watched their baby or toddler go through a severe allergic reaction.
Key findings include:
Skin changes, swelling, vomiting, and diarrhea were the most common signs
Some of the most serious signs—skin turning pale or blue-grey, or suddenly going limp—were often missed
About half of the caregivers noticed something was wrong during the reaction, but only understood it was an allergic reaction after the fact
Babies have gastrointestinal symptoms—like vomiting or diarrhea—more often than older kids or adults during a bad allergic reaction
Breathing problems are serious when they happen, but they're less common in babies than in older children
The study also found that the guidelines doctors and caregivers typically use to recognize anaphylaxis were written with older children and adults in mind—not babies. This matters because anaphylaxis can look different in infants than it does in older kids. On top of that, some symptoms of anaphylaxis in babies (like fussiness or vomiting) can also be signs of common illnesses in babies, which makes them easy to miss.
Common Triggers of Allergic Reactions in Babies
Food Allergens
For babies under 12 months of age, egg and cow's milk are the most common food allergens, followed by peanut, sesame, wheat, and tree nuts like almond, cashew, hazelnut, and pecan. While food is the most common trigger of food allergens in babies, most babies and toddlers do not have food allergies, and will never experience an allergic reaction. You can help prevent food allergies from developing by safely introducing allergens early on when starting solids and regularly keeping them in the diet.
For babies who are allergic to a food, a severe allergic reaction (anaphylaxis) is very unlikely the very first time they taste the food allergen. That's because the body's immune system needs to encounter the food at least once before it can build up a strong enough reaction to cause a dangerous response. However, small, unnoticed exposures—like repeated skin exposure to the allergen residue from the hands of a caregiver (especially if baby has eczema), can silently make the immune system more sensitive over time. This is why a severe reaction can sometimes seem to come out of nowhere.
Medications
Certain medications can trigger allergic reactions in babies. Penicillin-based antibiotics—including amoxicillin, one of the most commonly prescribed antibiotics in early childhood—are among the most recognized medication triggers. If baby is being prescribed an antibiotic for the first time, get familiar with the symptoms of an allergic reaction and pay close attention after the first few doses. Allergic reactions to medications typically appear within the first few doses, not when the course of medication is nearly complete. Keep in mind that most rashes that appear while a baby is on an antibiotic are related to the illness itself, and not due to a drug allergy.
Insect Stings and Latex
Insect stings (such as bees, hornets, wasps, yellow jackets, and fire ants) and latex are less common triggers of allergic reactions in infants than food or medications, but both are recognized causes. Babies with a known latex allergy may need to avoid latex-containing medical equipment, like latex gloves, rubber catheters, or certain bandages.
Critical info for caregivers
Should you or your caregivers need to call emergency services, things will move more quickly if you have the following information readily available. Enter it in your own phone and post it on your refrigerator for caregivers.
Birth date
Weight
Address
Insurance card (photo of, copy of)
Nearest hospital (or preferred hospital)
Special health info (e.g., baby was born prematurely at 30 weeks, etc.)
Eczema Flare-up vs. Allergic Reaction vs. Contact Rash
An eczema flare-up, an allergic reaction, and a contact rash can all involve itchy, inflamed skin, which can confuse parents on what to do next. Yet knowing the difference between them can help you respond quickly if needed, or can prevent an unnecessary elimination of food from your child’s diet which can sometimes increase the risk of an allergy developing, rather than reduce it. So how can you tell the difference?
Start by examining the skin: if the rash is widespread (such as all over the torso, arms, and legs), it is more likely to be an allergic reaction and you should seek immediate medical guidance, especially if there are other symptoms of an allergic reaction. If you are not sure, it is always reasonable to seek medical guidance rather than waiting.
What's The Difference? Eczema vs. Allergy vs. Contact Rash
Category | Eczema Flare-Up | Classic Allergic Reaction* | Contact Rash |
|---|---|---|---|
What It Often Looks Like | rough, bumpy, intensely itchy patches often with multiple scratches | hives (often pale in the center and red or purple around the edges) and/or swelling of the lips or eyes | red or purple skin discoloration, not usually very itchy, sometimes with small bumps |
Timing | usually develops hours after exposure to a trigger or irritant | usually appears a few minutes (but can appear up to 2 hours) after eating | appears a few minutes after skin touches food |
Area Affected | shows up where skin is sensitive (cheeks, skin folds) and persists for a few days or longer | hives can be widespread (present on skin that did not touch food) and can move around the body | limited to where skin touches food: hands, chin, mouth, neck (from drool) |
Duration | lasts for days to weeks and changes in severity over time, and generally improves with regular treatment | fades within a few hours without treatment (hives can fade within minutes if treated, swelling takes longer) | fades within 10 minutes or so after a gentle cleanse |
Other Symptoms | no other symptoms suggestive of an allergic reaction | other symptoms frequently appear, like face swelling, vomiting/diarrhea, lethargy, coughing, or trouble breathing | no other symptoms suggestive of an allergic reaction |
* For IgE-mediated allergies. Symptoms of allergic reactions vary depending on the type of allergy. Check out FPIES in Babies for symptoms of delayed allergic reaction, which are less common.
An eczema flare-up usually develops more slowly and tends to show up in areas where the skin is already sensitive, such as the creases of the elbows or knees, wrists, ankles, neck, or cheeks, and the skin often looks dry, rough, or scaly and may thicken over time from scratching. The flare can last days to weeks and is often triggered by things like dry air, sweating, stress, illness, or irritating soaps rather than a single allergen exposure.
An allergic reaction to food usually appears suddenly (within minutes to hours after contact with an allergenic food) and often causes raised, smooth, itchy bumps (hives) or swelling that can move around the body and fade within hours. Allergic reactions are also more likely to come with other symptoms, such as lip or eyelid swelling, vomiting, coughing, or trouble breathing, which are not features of eczema.
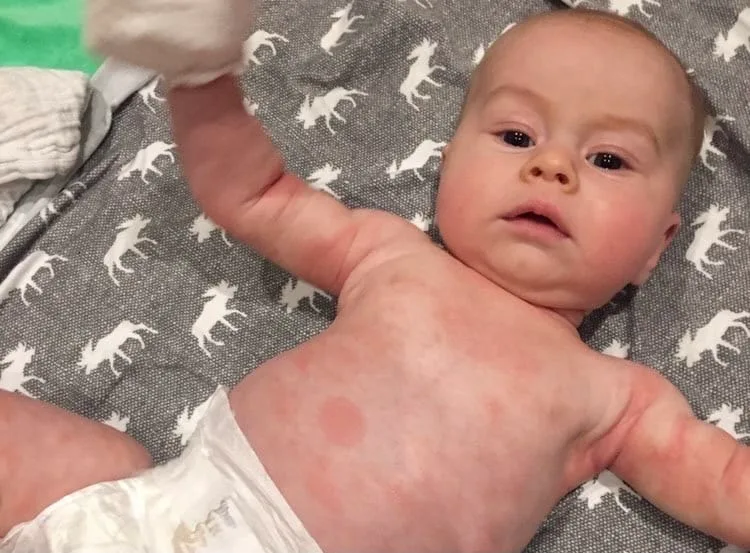
Contact rashes from acidic foods (such as lemon, orange, pineapple, and tomato) usually show up in a limited area where your baby’s skin came in contact with food, such as around the mouth and on the chin. Contact rashes typically dissipate within 10 minutes of a gentle cleanse, and there tend to be no other symptoms. If the rash does not resolve quickly after gentle cleansing, call your doctor for guidance. There is a chance that the reaction might become more serious if left untreated.
When in doubt, discuss with your baby’s healthcare provider. To offer them the most information possible, make sure to document the following information:
What food was served and the quantity consumed.
What time food was served.
Time of onset of symptoms and what was observed.
If a rash develops, take a picture and continue to document with more pictures if noting any changes to rash (worsening or improvement) and timing.
What to Do If Baby Shows Signs of A Severe Reaction
Step 1: Give Epinephrine First and Fast
Early use of epinephrine is one of the most important factors in preventing a reaction from becoming life-threatening. Delaying or failing to use epinephrine can make things worse.
If epinephrine has been prescribed for baby, give it immediately at the first sign of suspected anaphylaxis—do not wait for symptoms to worsen.
If you suspect anaphylaxis but don’t have epinephrine available, call emergency services right away and request an ambulance with epinephrine on board.
If you are not certain whether what you are seeing is anaphylaxis, it is okay to give the epinephrine anyway. The risk of giving epinephrine when it was not strictly needed is far smaller than the risk of withholding it during a true reaction.
Step 2: How to Administer an EpiPen
If baby is at risk of anaphylaxis and has been prescribed epinephrine, your doctor will explain how to use the specific epinephrine device that has been prescribed. Make sure every caregiver who spends time with baby is familiar with your prescribed device.
General steps for most auto-injectors:
Remove the auto-injector from its carrier/protective sleeve and take off any safety cap
Hold the device firmly in your dominant hand with the injection-end pointed down
Place baby on a firm surface or hold them securely on your lap
Position and push the auto-injector into the outer mid-thigh (can go through clothing)
Hold firmly against the thigh for the time specified on the device (typically 2–10 seconds)
Lift the device up from the thigh and note the time of injection for your records
For babies and toddlers who weigh less than 33 lbs (15 kg), either the 0.1 mg or the 0.15 mg epinephrine auto-injector dose may be appropriate. Your doctor will advise which has been prescribed and why.
Step 3: Call Emergency Services
Call emergency services immediately if epinephrine is not available, or if baby's symptoms are not improving after the first dose of epinephrine. Do not wait to see if things get better on their own.
If baby's symptoms resolve quickly and completely after epinephrine, current guidance allows for home observation in some situations—but for babies, this decision requires extra caution. Because baby cannot tell you how they feel, and because some serious signs can be subtle or appear after an initial recovery, the safest choice when you are unsure is always to call emergency services.
Call emergency services right away if:
Symptoms are not improving, or are getting worse
Baby is having difficulty breathing, making unusual sounds, or has a hoarse cry
Baby has vomited more than twice in total
Baby seems limp, unresponsive, or has pale, bluish, or mottled skin
Symptoms come back after initially improving
You do not have a second epinephrine auto-injector on hand
You are alone with baby
You may watch closely at home while staying ready to call emergency services if:
Baby's severe symptoms have resolved completely and quickly after epinephrine
Baby seems back to their usual self
You have a second epinephrine auto-injector immediately available
Another adult is with you
You are prepared to call emergency services the moment anything changes
Even when baby appears to have fully recovered, a second wave of symptoms—called a biphasic reaction—can occur hours later. See Step 5 for more on this.
Step 4. Position Baby for Safety
Unless baby is having trouble breathing, lay them on their back with legs elevated.
If baby is having difficulty breathing, keep them in the position that makes breathing easiest, usually semi-upright.
If baby loses consciousness, place them on their side. Never leave baby unattended.
Step 5: Watch for A Second Wave
A biphasic reaction is a second wave of anaphylaxis symptoms that can occur up to 72 hours after the initial reaction has resolved—without any further allergen exposure. However, the vast majority of biphasic reactions appear within the first 8 hours after anaphylaxis has resolved. Biphasic reactions are unpredictable and can range from mild to severe.
This is one of the key reasons why emergency department evaluation is recommended after an anaphylactic reaction, particularly when symptoms were severe or did not resolve quickly after a single dose of epinephrine.
Always have two epinephrine auto-injectors available. If symptoms return or do not fully resolve after the first dose, a second dose may be needed.
Step 6: Follow-Up After a Reaction
After any episode of anaphylaxis, follow-up with a board-certified allergist is important.
Your allergist can:
Confirm the diagnosis and identify the trigger if it was not already known
Review and update your Allergy and Anaphylaxis Emergency Care Plan
Ensure the correct epinephrine auto-injector has been prescribed
Help you ensure that all caregivers know how to use the auto-injector
Discuss longer-term management, including whether allergy testing or an oral food challenge is appropriate
Why An Anaphylaxis Action Plan Saves Lives
An Allergy and Anaphylaxis Emergency Care Plan is a written document, prepared with your allergist, that specifies which allergens to avoid, which symptoms require epinephrine, how to use the auto-injector, and when to call emergency services.
Every caregiver who spends time with baby— family members, caregivers, nursery staff—should have access to a copy of your plan and know how to follow it.
Research shows that children with a diagnosed food allergy who had an emergency care plan in place were significantly more likely to receive epinephrine during a severe reaction than those without one. When seconds matter, a clear written plan removes hesitation.
Ready to get started?
Download the app to start your journey.
Expert Tips Delivered to Your Inbox
Sign up for weekly tips, recipes and more.
Copyright © 2026 • Solid Starts Inc
