Allergy Symptoms in Babies
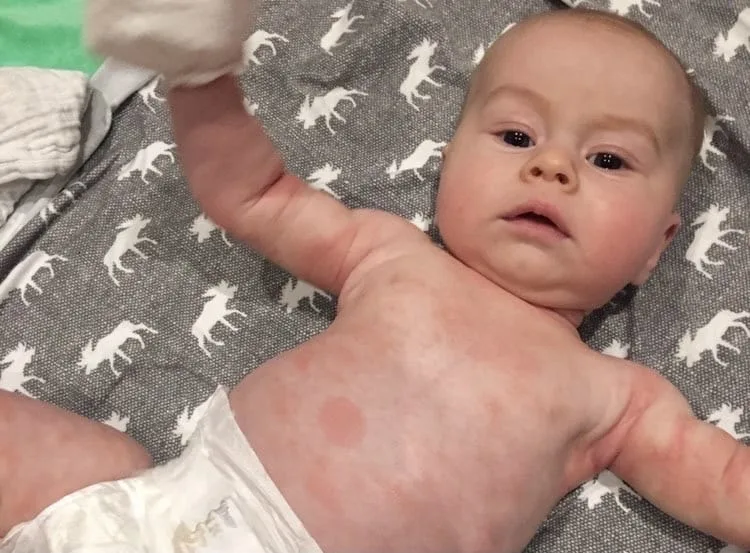
Spotting the signs of an allergic reaction early is important yet many parents do not know what symptoms are concerning and what is normal. Our pediatric pros explain the signs to look out for, share images of reactions, and offer guidance on what to do if an allergic reaction occurs.
Looking for a step-by-step guide to introducing allergens? The Solid Starts App can help. Start your free trial.
Key Points
✔ Allergic reactions vary in severity
Some reactions are mild, while others are life-threatening. The severity is judged by how many symptoms are present and the severity of those symptoms. The more allergen consumed, the more severe the symptoms may be.
✔ Symptoms vary, but there are common signs
Itchy mouth or nose, sneezing, hives are some examples of common allergic reaction symptoms in babies, but there are more. Review the full list below before you get started.
✔ Allergic reactions need immediate action
Most children will never experience an allergic reaction, but it can happen—and it is important to understand how to spot an allergic reaction and how to take action if it happens.
Symptoms of Food Allergies in Babies
Symptoms vary and range from mild to severe. Generally, the severity of a reaction is judged by how many symptoms are present and the severity of those symptoms.
If you think baby is having an allergic reaction, call emergency services immediately.
Symptoms of Allergic Reaction in Babies | |
Mild Reaction: includes one symptom (more than one is a severe reaction) | |
itchy or runny nose | |
itchy mouth | |
a few isolated hives, mild itching | |
mild nausea or gastrointestinal discomfort, a single episode of vomiting | |
Severe Reaction: includes any of the following, either alone or in combination with any other symptom | |
shortness of breath, wheezing, stridor (a whistling sound upon breathing in), repetitive cough | |
excessive drooling | |
pale, ashen or bluish skin | |
swelling of face, lips, or tongue | |
widespread hives or rash on body | |
repetitive vomiting or diarrhea | |
sudden tiredness/lethargy/seeming limp |
Mild Reaction
Includes ONE of the following (more than one is a severe reaction):
Itchy or runny nose, sneezing
Itchy mouth
A few isolated hives, mild itching
Mild nausea or gastrointestinal discomfort, or a single episode of vomiting
If you note any of the above symptoms, stop feeding the allergen and contact your pediatrician, family practitioner, or allergist for guidance. If your child is having multiple symptoms, call 9-1-1/local emergency services immediately and request an ambulance equipped with epinephrine.


Severe Reaction
Includes any of the following, either alone or in combination:
Shortness of breath, wheezing, stridor (a whistling sound upon breathing in), repetitive cough
Excessive drooling
Pale, ashen or bluish skin
Swelling of face, lips, or tongue
Widespread hives or rash on body
Repetitive vomiting or diarrhea
Sudden tiredness/lethargy/seeming limp
If your child is having any of the above symptoms, call 9-1-1/local emergency services immediately and request an ambulance equipped with epinephrine. Do not wait.









Delayed Reactions
Most allergic reactions occur within minutes of eating, though delayed reactions that occur several hours later are possible with FPIES, an increasingly recognized food allergy in babies and young children. It is often challenging to confirm an FPIES allergic reaction without the support of your doctor and a pediatric allergist or gastroenterologist because the most common symptoms are vomiting and diarrhea, which are common reactions to a number of childhood illnesses. Check out FPIES in Babies for more information.
A baby may not have an allergic reaction the first time they are exposed to the food, so be watchful on the second and the first few subsequent exposures. Generally, the more of the allergen consumed, the more severe the reaction is likely to be, so it is important to start small when introducing new foods and gradually work up to larger quantities served at mealtime.
Critical info for caregivers
Should you or your caregivers need to call emergency services, things will move more quickly if you have the following information readily available. Enter it in your own phone and post it on your refrigerator for caregivers.
Birth date
Weight
Address
Insurance card (photo of, copy of)
Nearest hospital (or preferred hospital)
Special health info (e.g., baby was born prematurely at 30 weeks, etc.)
Eczema Flare-up vs. Allergic Reaction vs. Contact Rash
An eczema flare-up, an allergic reaction, and a contact rash can all involve itchy, inflamed skin, which can confuse parents on what to do next. Yet knowing the difference between them can help you respond quickly if needed, or can prevent an unnecessary elimination of food from your child’s diet which can sometimes increase the risk of an allergy developing, rather than reduce it. So how can you tell the difference?
Start by examining the skin: if the rash is widespread (such as all over the torso, arms, and legs), it is more likely to be an allergic reaction and you should seek immediate medical guidance, especially if there are other symptoms of an allergic reaction. If you are not sure, it is always reasonable to seek medical guidance rather than waiting.
What's The Difference? Eczema vs. Allergy vs. Contact Rash | |||
| Eczema Flare-Up | Classic Allergic Reaction* | Contact Rash |
What It Often Looks Like | rough, bumpy, intensely itchy patches often with multiple scratches | hives (often pale in the center and red or purple around the edges) and/or swelling of the lips or eyes | red or purple skin discoloration, not usually very itchy, sometimes with small bumps |
Timing | usually develops hours after exposure to a trigger or irritant | usually appears a few minutes (but can appear up to 2 hours) after eating | appears a few minutes after skin touches food |
Area Affected | shows up where skin is sensitive (cheeks, skin folds) and persists for a few days or longer | hives can be widespread (present on skin that did not touch food) and can move around the body | limited to where skin touches food: hands, chin, mouth, neck (from drool) |
Duration | lasts for days to weeks and changes in severity over time, and generally improves with regular treatment | fades within a few hours without treatment (hives can fade within minutes if treated, swelling takes longer) | fades within 10 minutes or so after a gentle cleanse |
Other Symptoms | no other symptoms suggestive of an allergic reaction | other symptoms frequently appear, like face swelling, vomiting/diarrhea, lethargy, coughing, or trouble breathing | no other symptoms suggestive of an allergic reaction |
* For IgE-mediated allergies. Symptoms of allergic reactions vary depending on the type of allergy. Check out FPIES in Babies for symptoms of delayed allergic reaction, which are less common. |
An eczema flare-up usually develops more slowly and tends to show up in areas where the skin is already sensitive, such as the creases of the elbows or knees, wrists, ankles, neck, or cheeks, and the skin often looks dry, rough, or scaly and may thicken over time from scratching. The flare can last days to weeks and is often triggered by things like dry air, sweating, stress, illness, or irritating soaps rather than a single allergen exposure.
An allergic reaction to food usually appears suddenly (within minutes to hours after contact with an allergenic food) and often causes raised, smooth, itchy bumps (hives) or swelling that can move around the body and fade within hours. Allergic reactions are also more likely to come with other symptoms, such as lip or eyelid swelling, vomiting, coughing, or trouble breathing, which are not features of eczema.
Contact rashes from acidic foods (such as lemon, orange, pineapple, and tomato) usually show up in a limited area where your baby’s skin came in contact with food, such as around the mouth and on the chin. Contact rashes typically dissipate within 10 minutes of a gentle cleanse, and there tend to be no other symptoms. If the rash does not resolve quickly after gentle cleansing, call your doctor for guidance. There is a chance that the reaction might become more serious if left untreated.
When in doubt, discuss with your baby’s healthcare provider. To offer them the most information possible, make sure to document the following information:
What food was served and the quantity consumed.
What time food was served.
Time of onset of symptoms and what was observed.
If a rash develops, take a picture and continue to document with more pictures if noting any changes to rash (worsening or improvement) and timing.
Frequently Asked Questions
How long does it take for an allergic reaction to show up in babies?
Classic allergic reactions to food (IgE-mediated) typically occur within minutes of consuming the allergenic food, but can take up to 2 hours to appear. While most allergic reactions are immediate, a small percentage of babies may experience delayed gastrointestinal allergic reactions, typically due to FPIES.
How to tell if your baby had an allergic reaction?
Symptoms of an allergic reaction can vary depending on the amount of allergen ingested, if there was other food in the belly before the exposure, and the baseline health status of the child. Mild symptoms include itching of the mouth, a rash around the mouth, isolated hives, a runny nose, or minor tummy upset. Severe symptoms can include excessive drooling, trouble breathing, widespread rash/hives/itching, swelling, repetitive vomiting, or mental status changes.
What if I think baby had an allergic reaction but I’m not sure?
Stop serving the food for now and talk to your doctor. They can help you confirm if the reaction is due to a food allergy or something else. It’s important to have this conversation before jumping to the conclusion that you should avoid the food entirely. Unnecessary elimination of food from your child’s diet can sometimes increase the risk of an allergy developing, rather than reduce it.
Can allergies cause diarrhea in babies?
Yes. An allergic reaction to food may result in loose stools or even persistent watery diarrhea in more severe cases. However, when diarrhea is associated with an allergy, there are usually other signs, such as vomiting, blood in the stool, poor weight gain, or skin rashes, for example. The consistency of a baby’s poop can frequently change as their gut matures and learns to digest food, so loose stools in a baby who is otherwise happy and thriving are not typically due to a food allergy.
What does food allergy poop look like?
Many babies with food allergies don’t show any changes in their poop. When food allergy does affect bowel movements, common signs are streaks or globs of red blood, occasionally accompanied by large amounts of mucous. Persistent watery diarrhea can also be seen in food allergy, especially if the baby is consuming the allergen regularly. Small amounts of mucous, greenish colored poop, or short-lived watery poop in an otherwise thriving baby are not signs of allergy.
Can you give a baby Benadryl for allergic reactions?
It is not usually the best choice. Benadryl (diphenhydramine) is an older antihistamine that can cause babies to become very lethargic, which is not ideal during an allergic reaction. For mild allergic reactions, pediatric allergy specialists prefer non-sedating antihistamines that also act quickly (such as cetirizine). However, if your baby is experiencing a severe allergic reaction, antihistamines are not sufficient to reverse the reaction. If you suspect a severe reaction, call emergency services immediately and request an ambulance with epinephrine (adrenaline) on board
How to administer epinephrine to babies & toddlers?
How to administer epinephrine to babies
Written By
S. Bajowala, MD, FAAAAI. Board-Certified Allergist & Immunologist
K. Rappaport, OTR/L, MS, SCFES, IBCLC, Feeding and Swallowing Specialist
Ready to get started?
Download the app to start your journey.
Get 10% Off
Sign up to save and get weekly tips, recipes and more.
Copyright © 2026 • Solid Starts Inc
